Understanding NeuroCOVID-19: SARS-CoV-2 Disrupts Astrocyte Homeostatic Functions
Quantitative cellular analysis of COVID-19-infected astrocyte cells reveals a more central role of astrocytes in NeuroCOVID-19 and the interruptive impact of SARS-CoV-2 on astrocyte homeostasis capabilities, reframing astrocytes as active protagonists.
fluorescence
single-cell analysis
neuroscience
White Paper

Understanding NeuroCOVID-19: SARS-CoV-2 Disrupts Astrocyte Homeostatic Functions
30 Mar, 2026
Neuro- and Long COVID
In addition to its well-known respiratory symptoms, COVID-19 has more recently been recognized as a systemic illness with wide-ranging effects - including notable neurological impacts. Symptoms such as reduction or loss of taste (hypo/ageusia) and smell (hypo/anosmia), headaches, fatigue, seizures, brain fog, hallucinations, and strokes have been widely reported during the acute phase of infection. However, many of these neurological issues can linger for months (1).
This ongoing symptomatology has led to the condition now being referred to as Neuro-COVID-19. Research suggests that SARS-CoV-2 is neurotropic, capable of infecting neural tissue directly and accumulating over time. This persistent involvement of the nervous system is considered a key contributor to what is now known as Long COVID (2,3).
Although extensive research has been conducted to understand the impact of SARS-CoV-2 on neurons and microglia in relation to neural dysfunctions, astrocytes have received little attention. This is somewhat surprising given the critical role astrocytes play in maintaining central nervous system (CNS) homeostasis through neurotransmitter synthesis and reuptake, as well as regulation of cerebral blood flow. They are also often the first CNS cells to respond to viral infections, triggering immune responses via cytokine production. This can lead to neuroinflammation, cell death, and long-term neurological complications (4).
A recent study published in Brain, Behavior, & Immunity - Health, therefore, aimed to address this gap in the literature by investigating the prevalence of some of the neurological symptoms mentioned above in a Brazilian cohort, whilst examining how SARS-CoV-2 disturbs human-induced pluripotent stem cell (hiPSC)-derived cortical astrocyte function.
Neurological Symptoms Displayed in a Brazilian COVID Infected Cohort
Over half of the Brazilian cohort in the study reported at least one of the assessed neurological symptoms: asthenia, brain fog, olfactory and gustatory agnosia, and headache.
The most prevalent symptoms reported among all positive-tested individuals in the screening were headaches (53%), brain fog (42%), and anosmia (39%) (5).
The impact of COVID-19 on Astrocytes
After assessing the frequent neurological symptoms exhibited by the Brazilian cohort of COVID-19 patients, the researchers examined whether SARS-CoV-2 infection of cortical astrocytes leads to neuroinflammation, vasoregulatory disruption, glutamatergic imbalance, and apoptosis as potential pathogenic processes.
Immunofluorescence assay quantification was conducted on SARS-CoV-2-infected cortical astrocytes, and the cortical astrocyte culture was stained for GFAP (astrocyte marker), Casp3 (apoptosis marker), and SARS-CoV-2. The stained well plate cultures were imaged using TissueGnostics’ versatile imaging platform, TissueFAXS scanning microscope, and analyzed using StrataQuest, an image analysis solution. The quantitative image analysis allowed to show the colocalization of viral and astrocytic markers, suggesting that the virus is capable of entering astrocytes, likely using the same cellular entry receptors described for neural progenitor cells (NPC) and neurons. Although SARS-CoV-2 did not result in clear cytopathic effects in hiPSC astrocytes, a significant increase in cleaved caspase-3 expression was detected in infected cells.
Multi-analyte profiling analysis revealed elevated levels of IL-6, IL-15, and IL-4 in the culture supernatant, indicating that a pronounced proinflammatory response is exhibited when astrocytes are infected with SARS-CoV-2 (5).
Infected astrocyte cells also displayed reduced mRNA expression of KLK1 and EAAT1 genes, which are fundamental in vasodilation and glutamate clearance, respectively (5).
Together, these findings reveal that SARS-CoV-2 directly disrupts astrocyte function, leading to neuroinflammation, dysregulation of excitatory neurotransmission, and cell death. Thus, the study further validates the gliotropic nature of the virus, and its possible contribution to the onset of Neuro-COVID, whilst also highlighting the role of astrocytes in CNS vulnerability (5).
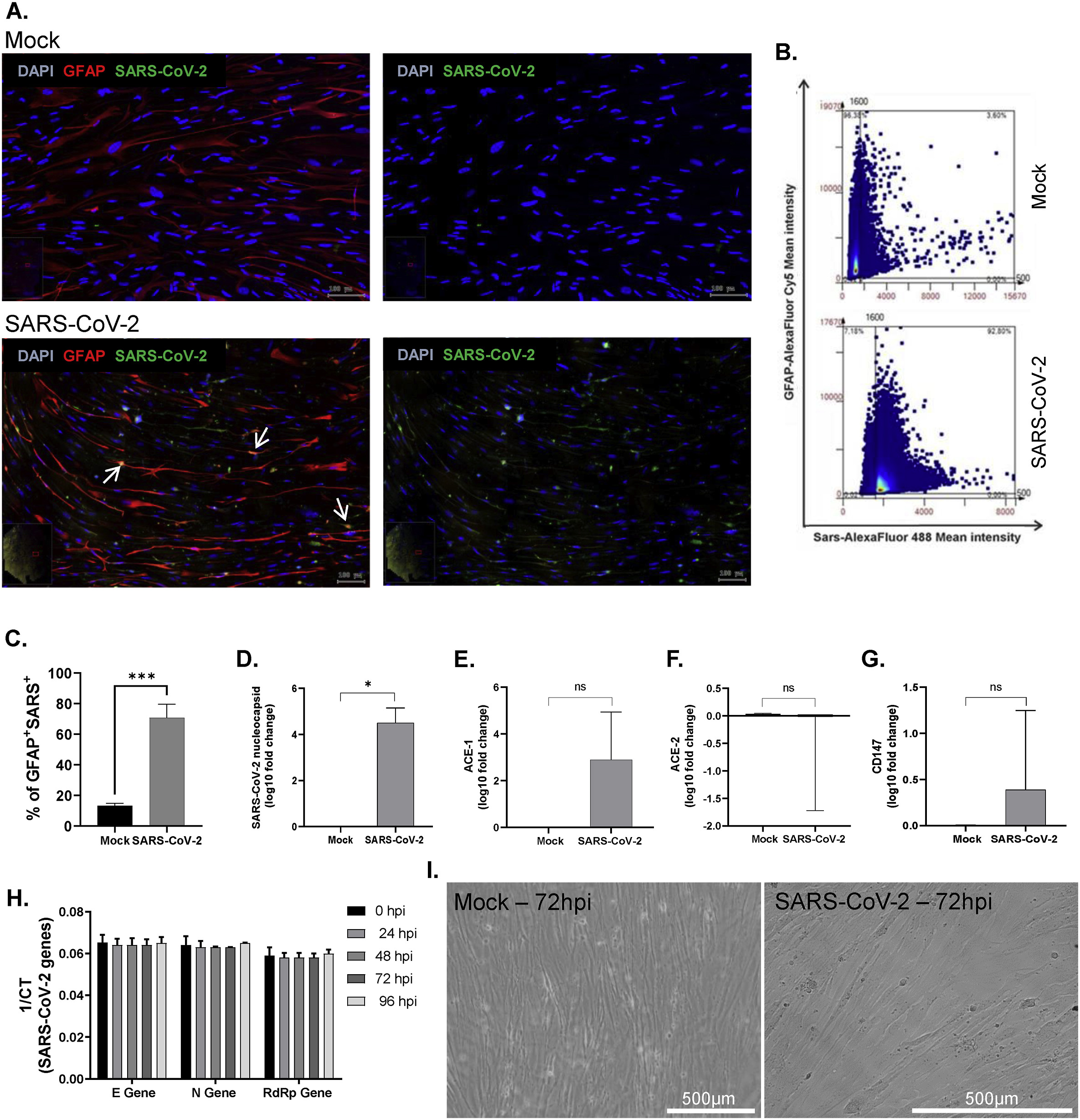
Adapted from Astroglia-mediated neuroinflammation as a putative mechanism of neurological outcomes in COVID-19? Insights from a Brazilian cohort by Segabinazi et al, 2026. Figure 2. SARS-CoV-2 gliotropism on cortical astrocytes derived from hiPSCs.
Linking Cohort Symptoms to COVID-19 Impacts on Astrocytes
Astrocyte apoptosis, marked by increased expression of cleaved caspase-3, was observed even in the absence of productive infection, and appears to be driven by a pro-inflammatory response, particularly through elevated secretion of cytokines such as IL-4, IL-6, and IL-15 (5). Although in line with the canonical role of astrocytes, this innate antiviral response can become maladaptive if long-lasting, causing local neuroinflammation and cell death in astrocytes and even neighboring neurons (4).
This inflammatory environment could well exacerbate the cognitive disturbances related to brain fog, as pro-inflammatory cytokines can decrease neurogenesis and synaptic plasticity, which are vital elements in correct cognitive function (5).
In this study, brain fog in the patient cohort may also be explained by several factors in play: inflammatory environment, vasoconstrictive effects and impaired glutamatergic signaling (5). Neuroinflammation and vasodilation, key downstream effects of astrocyte impairment, are known contributors to headache pathogenesis and can be intensified by excess glutamate. Glutamate-mediated excitotoxicity could therefore explain the high incidence of headaches reported in the study cohort (5).
The relationship between astroglia damage and Neuro-COVID-19 deficits could be more specifically determined through correlation of symptoms with the changes observed in astrocytes exposed to sera or derived from cohort participants (2).
According to the Brazilian research team, a deeper understanding of the cellular and molecular mechanisms behind SARS-CoV-2’s impact on the central nervous system is essential for identifying potential therapeutic targets and guiding the development of preventive strategies.
Conclusion
This study highlights the pivotal role astrocytes play in the neuropathological landscape of Neuro-COVID-19, showing how infection disrupts their homeostatic functions. In doing so, the findings point to potential therapeutic targets for addressing COVID-19-related neurological complications.
Quantitative image analysis remains a key tool for uncovering these cellular-level dynamics, providing critical insights into complex biological processes. To learn more about TissueGnostics’ imaging and analysis solutions, contact one of our experts today!
Resources
- Jin, X.I., Lian, J.S., Hu, J.H., Gao, J., Zheng, L., Zhang, Y.M., Hao, S.R., Jia, H.Y., Cai, H., Zhang, X.L. and Yu, G.D. 2020. Epidemiological, clinical and virological characteristics of 74 cases of coronavirus-infected disease 2019 (COVID-19) with gastrointestinal symptoms. Gut. 69(6), pp.1002-1009.
- Cheng, J., Zhao, Y., Xu, G., Zhang, K., Jia, W., Sun, Y., Zhao, J., Xue, J., Hu, Y. and Zhang, G. 2019. The S2 subunit of QX-type infectious bronchitis coronavirus spike protein is an essential determinant of neurotropism. Viruses. 11(10), p.972.
- Geng, L.N., Erlandson, K.M., Hornig, M., Letts, R., Selvaggi, C., Ashktorab, H., Atieh, O., Bartram, L., Brim, H., Brosnahan, S.B. and Brown, J. 2025. 2024 update of the RECOVER-adult long COVID research index. Jama. 333(8), pp.694-700.
- Jorgačevski, J. and Potokar, M. 2023. Immune functions of astrocytes in viral neuroinfections. International Journal of Molecular Sciences. 24(4), p.3514.
- Segabinazi, E., Tocantins, F.R., Glaser, T., Maglio, T., Oliveira, N.C., Castanha, A.G., Russo, F.B., Leite, P.E.C., Brito, A., Molina, C.V. and Paludo, G.P. 2025. Astroglia-mediated neuroinflammation as a putative mechanism of neurological outcomes in COVID-19? Insights from a Brazilian cohort. Brain, Behavior, & Immunity-Health. p.101115.

